Disclosure: I am compensated for purchases made through some links on this site. Click for details.
What is Gastroesophageal Reflux Disease (GERD)?
Gastroesophageal reflux disease (GERD) is the chronic occurrence of acid reflux, meaning two or more times a week. The most common symptom of GERD is the pain of heartburn caused by refluxed acid irritating the esophagus.
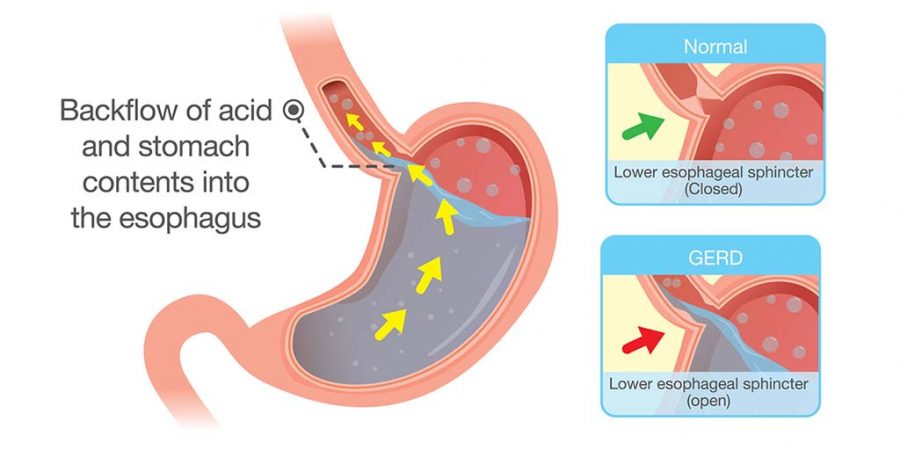
Acid reflux occurs when a ring of muscle at the base of the esophagus, called the lower esophageal sphincter (LES), fails to close properly. When the LES is compromised, acid can back up from the stomach (reflux) into the esophagus and cause irritation.1
How Common is GERD?
GERD is the third most common gastrointestinal disorder in the U.S. affecting approximately 20% of Americans.2
Symptoms of GERD
The symptoms of GERD are:3
- Heartburn
- Excessive saliva
- Bitter taste
- Bloating
- Burping
- Hiccups
- Nausea
- Vomiting
- Bad breath
- Dental erosion
- Laryngitis
- Hoarseness
- Trouble swallowing
- Sore throat
- Cough
- Pneumonia
- Asthma
- Weight loss
- Bloody stools or vomit
GERD is caused by chronic acid reflux. Please see Acid Reflux Symptoms for more symptom details.
Causes of GERD
There are numerous causes of GERD. The following are top factors contributing to chronic acid reflux.
- Heartburn trigger foods
- Caffeine
- Alcohol
- A diet low in fiber
- Pressure placed on the abdomen
- Overeating
- Being overweight
- Being pregnant
- Smoke from cigarettes (active or passive)
- Nicotine
- Eating before bedtime
- Medications that compromise the function of the LES
- Hiatal hernia
- Stress levels
- Hypochlorhydria (low stomach acid)
- Age
Diagnosis of GERD
If you have heartburn two or more times a week or at all concerned, it’s time to see a doctor about your condition, especially if you’ve also been treating the heartburn with OTC heartburn medications for more than two weeks.
Health providers interested in treating your underlying condition will likely discuss lifestyle and diet changes. If improvement isn’t obtained through lifestyle, diet, and GERD medications, your doctor my need to perform one or more tests to better evaluate and treat your condition.4
- Barium Swallow: In this test, liquid barium is swallowed and x-rays are taken. The barium allows the upper digestive tract to be highlighted for detection of esophageal and stomach abnormalities and to check for erosion, ulcers and narrowing of the esophagus due to scaring. This narrowing is called a stricture.
- Endoscopy: An endoscopy allows the doctor to visually check for problems in esophagus and stomach by running a flexible tube with camera down the esophagus.
- Biopsy: Tissue samples can be taken during an endoscopy to check for problems such as cancer.
- pH Monitoring: Acid levels in the esophagus can be checked by inserting a device into the esophagus for 1-2 days.
- Esophageal Manometry: During an esophageal manometry test a thin, pressure-sensitive tube is run through your nose, down the esophagus, and into the stomach to test the function of the LES and muscles in the esophagus.
Complications of GERD
Left untreated, GERD can lead to:3
- Esophagitis: Esophagitis is inflammation, irritation, or swelling of the esophageal lining.
- Esophageal Ulcer: An esophageal ulcer is a sore that can form from acid erosion of the esophageal lining. Esophageal ulcers may cause bleeding, pain, and difficulty swallowing.
- Esophageal Stricture: Stomach acid can cause scar tissue to form in the esophagus. This scar tissue can cause a narrowing of the esophagus is called a stricture. Esophageal strictures can cause swallowing difficulties. They are treated by stretching (dilatation) the narrowing in the esophagus.
- Barrett’s Esophagus: Barrett’s esophagus is a precancerous condition where repeated exposure to stomach acid changes the esophageal lining into tissue similar to that lining the intestines.
- Lung Conditions: Stomach acid can get into the lungs when refluxed to cause coughing, bronchitis, and pneumonia.
- Esophageal Cancer: There is a slightly higher risk of esophageal cancer in those with GERD, and even more so in those with esophagitis and Barrett’s esophagus.
Prevention of GERD
Changes in lifestyle and diet reduce or eliminate GERD. Some of these include:
- Improving diet.
- Not overeating.
- Eating 4 to 5 meals a day instead of the typical 2 or 3.
- Losing weight.
- Avoiding movement and clothing that might cause additional abdominal pressure. Abdominal pressure can compromise the LES allowing acid to reflux into the esophagus.
- Remain upright and maintain good posture after eating to reduce pressure on the LES.
- Improve digestive function. Slow digestion can lead to added pressure on the LES.
- Avoid nicotine.
- Avoid heartburn trigger foods.
- Establish an elimination diet if necessary to determine your heartburn trigger foods.
- Start a heartburn journal to help narrow down things that might cause you heartburn… food, activities, times, and any other relevant information should be documented.
- Fast 2 to 3 hours before bedtime.
- Elevating the torso while sleeping can reduce nighttime heartburn. Raise the head of the bed 6 to 8 inches with blocks, mattress bed wedge, or acid reflux pillow system to keep pressure off the LES.
- Certain medications can weaken the LES. Prohibiting it from closing properly. Your doctor should be consulted to see if the timing of these medications could be adjusted or if alternative medication might be appropriate.
Related Content:
- 8 Ways Nicotine Increases Heartburn
- E-Cigarettes and Heartburn Connection
- Elevation Therapy For Heartburn At Night: Time To Sleep On An Incline
Treatment for GERD
Most people can overcome GERD through lifestyle and diet changes. Your doctor may help you manage the discomfort of GERD through medications. In some circumstances, surgery or other procedures may be needed.5
GERD Medications
Discuss GERD medications with your doctor before treating your symptoms. The following GERD medications do not treat GERD. They primarily mask the symptom of heartburn. Lifestyle, diet changes, and a time for healing from any damage caused by GERD are typically required. We are all different and your doctor can guide you through your best course of treatment.
Heartburn, acid reflux, and GERD medications have levels of aggression in fighting stomach acid. In order, they are antacids, H2 blockers, and PPIs.
Antacids
Antacids neutralize stomach acid. They are fast-acting and can provide relief for up to two hours. There are different options when seeking a choice of antacid. Some have a coating effect as added protection. Antacids with coating properties help protect the esophagus by forming a barrier against stomach acid.
Antacids include:
- Tums
- Alka-Seltzer
- Pepto-Bismol
- Rolaids
- Rennie
- Gaviscon
- Kaopectate
- Phillips’ Milk of Magnesia
- Mylanta
- Maalox
H2 Blockers
H2 blockers take a few hours before taking effect. They can provide up to twelve hours of relief by decreasing the production of acid the stomach produces.
H2 blockers include:
- Pepcid
- Tagamet
- Zantac
- Axid
Proton Pump Inhibitors (PPIs)
PPIs are the strongest acid suppressants. They are primarily used to lower stomach acid level to allow healing of damaged tissue in the esophagus.
PPIs are for short-term use as directed on the pharmaceutical label or prescribed by your doctor. Studies have linked PPIs to an increased risk of death, increased risk of heart attack, liver damage, and chronic kidney disease. The use of PPIs can also trigger a rebound of acid production on discontinuing use.
PPIs include:
- Prilosec
- Nexium
- Prevacid
- Zegerid
- Vimovo
- Rapinex
- Protonix
- Losec
- Kapidex
- Dexilant
- AcipHex
GERD Surgery
GERD surgery is considered if GERD medications, diet and lifestyle changes do not correct GERD. Two different surgical options for improving the function of the LES are the LINX device and fundoplication.
LINX Device: The LINX device is a ring of titanium beads held together by titanium wire. It is surgically placed around the lower end of the esophagus to mechanically strengthen the LES.6
Fundoplication: Fundoplication wraps the top part of the stomach around the LES to strengthen it.
Foods to Avoid with GERD
Some foods can cause increased problems with GERD. They cause irritation, increase acid in the stomach, and weaken the LES. These are considered to be heartburn trigger foods. Everyone is different and some foods may cause acid reflux in some people and not in others. Elimination diets can also help narrow down problem foods. Keeping a heartburn journal is also a help for narrowing down foods and events that trigger heartburn.
Some of the top heartburn trigger foods are:7
- Processed foods
- Fatty meat
- Fried food
- Dairy
- Spicy food
- Onions
- Tomatoes
- Acidic fruits
- Alcohol
- Coffee
- Caffeine
- Carbonated beverages
- Mint
- Chocolate

References
1) “Symptoms & Causes of GER & GERD.” The National Institute of Diabetes and Digestive and Kidney Diseases, November 2014.
2) Amy Wang, Nora C. Mattek, Jennifer L. Holub, David A. Lieberman, & Glenn M. Eisen. “Prevalence of Complicated Gastroesophageal Reflux Disease and Barrett’s Esophagus Among Racial Groups in a Multicenter Consortium.” National Center for Biotechnology Information, U.S. National Library of Medicine, Digestive Diseases and Sciences, March 3, 2009.
3) “Definition & Facts for GER & GERD.” The National Institute of Diabetes and Digestive and Kidney Diseases, November 2014.
4) “Diagnosis of GER & GERD.” The National Institute of Diabetes and Digestive and Kidney Diseases, November 2014.
5) “Treatment for GER & GERD.” The National Institute of Diabetes and Digestive and Kidney Diseases, November 2014.
6) Luigi Bonavina, Greta Saino, John C. Lipham, & Tom R. DeMeester. “LINX® Reflux Management System in chronic gastroesophageal reflux: a novel effective technology for restoring the natural barrier to reflux.” National Center for Biotechnology Information, U.S. National Library of Medicine, Therapeutic Advances in Gastroenterology, July 2013.
7) “Eating, Diet, & Nutrition for GER & GERD.” The National Institute of Diabetes and Digestive and Kidney Diseases, November 2014.